Monkeypox has been declared an international public health emergency by the World Health Organization. Although many will have never heard of monkeypox before this outbreak, the virus is thought to have infected people for centuries, perhaps even millennia. Two monkeypox outbreaks were reported in 1958 when lab monkey colonies were being kept for research-hence; its name-which belongs to the same virus family as chickenpox and smallpox.
A number of rodents are known to carry the virus, including squirrels, pouched rats, and dormice. Virus outbreaks tend to occur in tropical rainforests in Central and West Africa. There were nearly 4,600 suspected monkeypox cases in the Democratic Republic of Congo (DRC) alone in 2020, a 14-fold increase from the 1980s through 2010. Nigeria has also seen more than 550 suspected cases as of 2017.
In the U.S., more than 300 cases have been reported. Public health officials are likely undercounting cases since they cannot track all transmission chains. In order to prevent it from getting worse, it is important for everyone to know its symptoms, how it spreads, and the risks involved.
What is Monkeypox?
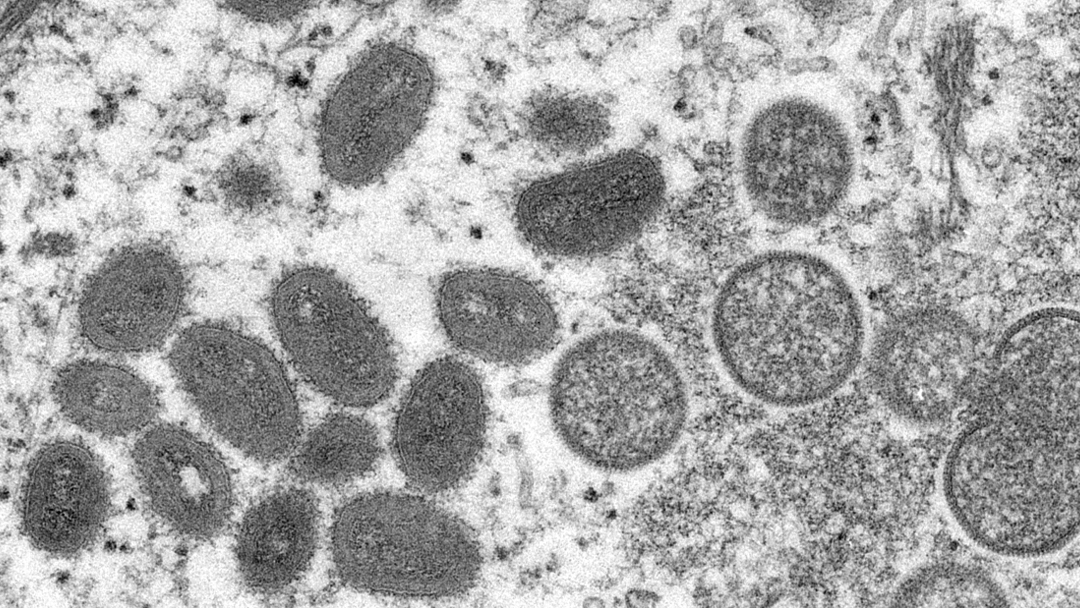
Except for the fact that they are viruses, monkeypox and chickenpox have no other similarities. Monkeypox, however, resembles smallpox, a disease that was eradicated by global vaccination in 1980. They are both orthopoxviruses. Unlike smallpox, monkeypox is not contagious or fatal. Researchers are concerned, however, that monkeypox may mutate and pose a greater threat to humans. According to one study published in 2008, monkeypox could become an epidemic if introduced to unvaccinated people.
Monkeypox was named after colonies of monkeys used for research. However, the Centers for Disease Control and Prevention do not believe it originated with animals because the source of the disease is unknown.
A single outbreak was detected in six states in 2003, with 47 confirmed and probable cases. The CDC said at the time that the outbreak was linked to prairie dogs which had come into contact with rodents including squirrels, mice, and rats that were infected nearby.
Is monkeypox a cause for concern?
Currently, monkeypox poses a low risk to the public. There is a noticeable spread among men who have sex with men, but it won’t be long until it spreads to others. According to the European Centre for Disease Prevention and Control, 10 women had been reported to the center as of June 27. There are several people who are susceptible to monkeypox. These include people with special medical conditions, pregnant women, fetuses or newborns, breastfeeding women, young children, and those with severe skin diseases like eczema.
However, if monkeypox spreads unchecked in the U.S. and around the globe, it could become endemic.
Monkeypox: how does it spread?
A close relative of smallpox, monkeypox is a viral infection. However, the disease is much milder.
Sexual contact, kissing, massage, or anything else that contacts the penis, vagina, anus, mouth, throat, or even skin can transmit it. There has been a major sexual transmission of monkeypox in the current outbreak.
Because condoms and dental dams protect only the skin and mucosa that they cover, they won’t prevent all transmission. In addition to entering broken skin, the virus can penetrate mucous membranes, including eyes, nostrils, mouths, genitalia, and anus. Vaginal fluid or semen might transmit monkeypox, but scientists aren’t sure.
A few feet away, monkeypox can be spread through respiratory droplets or “sprays,” but this mode of transmission is not thought to be particularly efficient. Although monkeypox has not been documented to spread through aerosols, as covid-19 does, it is possible. There is no consensus on whether monkeypox can be transmitted without symptoms.
Monkeypox Incubation Period
According to CDC study, the incubation period can range anywhere between five and 21 days between exposure and the onset of symptoms.
Symptoms of monkeypox
There are two distinct stages of monkeypox infection. A person’s immune system begins to fight off the infection as soon as the virus enters his or her cells, resulting in flu-like symptoms including
- exhaustion
- fever
- body aches
- chills
- headaches.
In the second stage, an unpleasant rash called “pox” develops. It usually begins on the face and spreads to the arms, legs, hands, feet, and trunk. A rash has been reported around the genital area in some of the patients in the latest outbreak.
Monkeypox isn’t instantaneous, so you shouldn’t assume you have it just because you have a rash. Also, genital rashes can indicate sexually transmitted infections such as herpes and chickenpox. There is a distinct monkeypox rash that begins flat and red, then blisters and fills with pus. Eventually, they become scabs, which fall off as they heal. Generally, the illness does not last more than two to four weeks and is not too serious.

How does the monkeypox rash look?
It is usually characterized by red spots that evolve into fluid-filled and then pus-filled bumps that may appear as blisters or pimples as the rash progresses. It then opens up into sores and scabs. Until the sores scab over and fall off, people with monkeypox should be considered contagious. And yes, monkeypox sores can be painful. There have been many cases of external and internal lesions of the mouth, genitalia, and anus in this outbreak, compared to the past when the rash was usually found on palms and soles. Additionally, people who have empty bowels may experience rectal pain or the sensation of needing to poop.
Is monkeypox deadly?
It’s good news that the West African type of monkeypox hasn’t proven to be extremely deadly. The CDC estimates that over 99% of patients will survive.
In most cases, monkeypox is mild and doesn’t require treatment. It is, however, capable of being lethal. There are between 1 and 3 percent fatalities associated with the West African strain responsible for the current outbreak. Congo Basin strains have a fatality rate of 10 percent.
Those with compromised immune systems, young children, pregnant women, or those who are breastfeeding are at greater risk of contracting an infection.
Scarring from an infection is the most common outcome. Despite this, monkeypox in humans can cause more serious complications, such as pulmonary distress and bronchopneumonia, according to research published in 2009.
A severe case of the virus can result in permanent vision loss due to corneal scarring and eye infections.
In what way does the Monkeypox virus spread?
Monkeypox is not common in the United States, but those who come into close contact with someone carrying the disease are at risk for infection, according to the CDC.
Human-to-human contact is the source of the current outbreak. A monkeypox carrier could transmit an infection if you spend too much time face-to-face with him or her, the WHO warns. Also, the virus can be spread physically through touching a lesion or exchanging bodily fluids such as saliva. If an individual touches items or surfaces shared with someone exhibiting symptoms, they may become infected.
Can I get monkeypox if I have been exposed to it?
Consult your health service if you have any questions and avoid contact with others. Vaccines may be offered along with self-isolation.
Is it possible to get monkeypox tested?
Go to your nearest sexual health clinic if you have symptoms of monkeypox, such as oral, genital, or anal lesions. Any suspicious lesion should be swabbed by a medical professional for testing. The U.S. health officials haven’t recommended throat swabs for screening monkeypox, although there’s emerging evidence they might be useful.
Does monkeypox have a vaccine?
Yes. Jynneos vaccine, Imvanex in Europe and ACAM2000 vaccine are effective against monkeypox. People 18 and older can use the Jynneos vaccine to prevent monkeypox and smallpox. FDA-approved ACAM2000 prevents smallpox. Due to its safety and fewer side effects, the U.S. currently uses only the Jynneos vaccine.
There is no risk associated with the Jynneos vaccine. The product has been tested on thousands of people, including immunocompromised patients and those with skin conditions. It is common for Jynneos vaccine recipients to experience side effects such as fever, fatigue, swollen glands, and injection site irritation.
Vaccination with Jynneos prevents monkeypox disease up to four days after exposure and may lessen symptoms if administered up to 14 days later.
Would I be able to get a monkeypox vaccination?
At present, the Centers for Disease Control and Prevention recommend monkeypox vaccination only for those at heightened risk:
- Close contacts with people who have monkeypox;
- Sexually active men and trans women in an area where monkeypox is spreading or where there was monkeypox recently;
- Personnel in the healthcare industry, laboratory staff, first responders, and members of the military who may come into contact with those affected.
A limited number of Jynneos vaccines are available at the moment. From the strategic national stockpile, the U.S. Department of Health and Human Services will release 56,000 doses right away. In the next few weeks, more than 1.5 million doses will be available, followed by 750,000 in the summer and 500,000 in the fall.
In the vaccine strategy, the goal is to interrupt transmission among MSM at highest risk by using post-exposure prophylaxis and pre-exposure prophylaxis.
Does monkeypox have a treatment?
There is no proven, safe treatment specifically for monkeypox. Monkeypox is usually mild and gets better without treatment after a couple of weeks. Fever and muscle pain can be treated with medications such as acetaminophen and ibuprofen, and pain can be treated with medications such as acetaminophen, ibuprofen, and opioids. A minority of patients will develop more severe illnesses and may require more specific treatment, for example, immunocompromised people, pregnant women, fetuses, newborns, breastfeeding women, children, and people with severe skin diseases.
ACAM2000 and Jynneos vaccines may also reduce the severity of the disease if administered early in the course of infection.
There are also antiviral drugs approved for treating monkeypox, such as TPOXX in the European Union, but none by the US FDA. Vaccine immune globulins, cidofovir, Brincidofovir and tecovirimat are among the experimental therapies being tested by US CDC. Laboratory tests have shown cidofovir to be effective against smallpox and other viruses of the same family.

What are the best ways to protect from monkeypox?
In situations where personal space cannot be maintained and bumping into others is impractical, the CDC advises people to exercise caution. Places such as raves and clubs, where clothing is minimal and you could come into contact with people, increase the risk.
The Centers for Disease Control and Prevention recommend keeping bedding, clothes, and towels away from potential sources of contamination until you can do a load of laundry. When you finish cleaning, be sure to wash all cleaning materials with soap and water and dispose of them.
Staying informed about the spread of the virus in your area is another way to keep yourself and your loved ones safe. Check the CDC’s map of monkeypox cases by state, or check the alerts published by state and local health departments.
Researchers are still trying to figure out whether monkeypox is present in feces, semen, and vaginal fluids even though it isn’t considered a sexually transmitted disease. You should inform your partner or partners that you may be exposed to the virus if you are sexually active.
In order to mitigate the risk of transmitting the virus to their newborns, pregnant carriers are advised to have C-sections before giving birth. Furthermore, preterm deliveries have been reported, as well as miscarriages and stillbirths.
In the event that I experience symptoms, what should I do?
These tips from the WHO can help if you experience the tell-tale symptoms:
- Make sure you don’t scratch your skin
- Maintain an uncovered and dry skin
- Use antiseptics or sterilized water to clean the skin
- Body lesions can be treated with baking soda or Epsom salts in a warm bath
- When treating mouth lesions, use saltwater rinses like you would when treating canker sores
- Shared households should isolate themselves in their rooms and, if possible, use designated bathrooms.
- Wash your own clothes, towels, and eating utensils.
- Ventilate your room whenever possible by opening the windows, but don’t sweep or vacuum, which can disturb virus particles on the floor.
Are there any misconceptions about monkeypox circulating?
Monkeypox is the subject of many conspiracy theories.
- There is no hoax about monkeypox — it is real.
- Monkeypox cannot be transmitted by Covid vaccines.
- Bill Gates and pharmaceutical companies did not invent monkeypox.
- The monkeypox virus did not originate in China or Ukraine.
- Monkeypox hasn’t been brought into the U.S. from Mexico by migrants.
- Monkeypox isn’t just a scheme to allow voters to mail in ballots. Monkeypox does not require a vaccine mandate or lockdowns.
Infected individuals should not be stigmatized. There are many falsehoods surrounding monkeypox, including that it affects only men who have sex with men or that it is caused by this group. Anyone can contract the disease, regardless of their gender or sexual preference.
Monkeypox Update around the globe.
Spain has seen a decrease in cases over the past few weeks, but the data may be incomplete because of reporting delays. Generally, females and children with epidemiological links to MSM have been reported only in major urban areas. HIV-positive people, their contacts, and health workers are getting pre-exposure prophylaxis with vaccines, however, vaccine supplies are low.
With 3,125 cases reported worldwide, Spain is next, followed by Germany with 2,352.
The United States reported 30 cases, while the United Kingdom reported 302 and Spain reported 198. UK has reported a few cases of monkeypox with serious symptoms (including encephalitis: Inflammation of the brain), and it plans to include proctitis (Inflammation of the anus) in its case definition of monkeypox. Observations in hospitals and households have revealed monkeypox virus DNA on surfaces (presumed infectious since the Ct value is moderate).
Most monkeypox cases in the United States occur in three large cities, but the disease is widely spread across the nation. 99% of cases involve male-to-male sexual contact, with a few cases occurring in children and in pregnant women.
A wide range of pre-exposure prophylaxis is being used in Canada, as 99% of cases have been reported among MSM. A strong focus is placed on engagement with community-led organizations serving key affected populations. A total of 681 monkeypox cases have been reported in Canada, making it the seventh most affected country.
In the period between September 2017 and July 2022, Nigeria recorded a little over 800 cases of monkeypox, with a case fatality rate of 3% among confirmed cases. In most cases, men between the ages of 31 and 40 are affected; no evidence of sexual transmission was found. It has been observed that the number of annual reported cases in 2022 is the highest since 2017.


Thanks for your blog, nice to read. Do not stop.